It was May 25, 2014 when the World Health Organization (WHO)
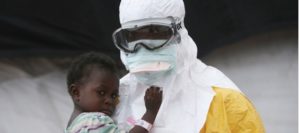
reported its first documented case of Ebola in Sierra Leone. Since then, other countries like Liberia, Guinea and Nigeria have been incessantly fighting the eradication of the deadly virus and preventing its spread to other countries, diminishing the risk of a world-wide pandemic. Today, after a hard fought battle, Ebola cases have significantly declined in Sierra Leone and Guinea, and Liberia and Nigeria are now Ebola-free. However, the fight to eradicate this deadly disease comes at a price for both Sierra Leone and Liberia; they both have tanking economies, staggeringly expensive healthcare systems, and rates of rising preventable illnesses neglected during the Ebola crisis.
Many working families have since been economically affected by the outbreak of Ebola. The height of the outbreak occurred during the farming season, making farmers some of the most affected by the deadly virus. In addition, strikes conducted by health workers in Liberia forced farmers to flee their land and threatened to bring the country’s food supply to a halt. Ebola not only debilitated their workforce, but also devastated their crops. Their farmlands have since become wastelands. Other measures taken to quell the spread, such as restricting trading hours and keeping citizens under quarantine during the night, diminished opportunities for citizens to conduct business with one another, catalyzing financial troubles.
The outbreak comes after decade-long civil wars in Sierra Leone and Liberia.

Since the end of their wars, both of these countries have struggled to keep commodities prices stable. Neither have been able to implement a healthcare infrastructure effective enough to react to rising rates of malnutrition, implement necessary HIV prevention measures, or effect required child immunizations. When Ebola surfaced these countries were making progress at piecing together their fragmented health systems by increasing immunizations in children and preventing citizens from malaria infection. However, The outbreak of Ebola not only exposed their lack of healthcare surveillance measures, but also the lack of resources needed to handle an endemic of this magnitude without neglecting other rising health issues. The rates of malnutrition, malaria infections, and infant mortality due to cholera, typhoid and other illnesses continue to rise. Ebola has drained their healthcare systems of resources necessary to deal with these illnesses. The progress that they had steadily seen in the last years quickly vanished. Doctors without Borders have reported more deaths due to Malaria than to Ebola since the outbreak.
As some of these countries continue to struggle to eradicate the Ebola virus, governments continue to suggest methods to improve their healthcare infrastructure and surveillance programs; however, resources are needed in order to train health workers and to build the facilities needed to detect dangerous diseases. The World Bank announced an additional $650 million toward rebuilding these Ebola affected countries. The World Bank continues to be the leading contributor to the fight against Ebola amongst International Institutions. The United Nations secretary-general, Ban Ki-moon, will hold a conference in July to get countries and institutions to pledge even more.
The road to recovery from this deadly disease that affected many countries around the world is slow and costly. The pledged resources will be used to build a healthcare system in these affected countries that will be resilient and can withstand the effects of a major endemic without collapsing the health system and economy. In addition, this system, with Liberia as its main developer, will be a model healthcare system for other developing countries in order to provide adequate response in a time of crisis by increasing trust, investing in the country and promoting growth.


